
On Tuesday, June 15, Solve M.E. President and CEO Oved Amitay joined other experts as a participant in the second seminar in a series presented by the World Health Organization (WHO) designed to improve our understanding of the Post COVID-19 condition and optimize the health of patients who have suffered from COVID-19.
In the first meeting on February 2, 2021, the WHO presented a framework that called for “Recognition; Research and Rehabilitation.” As part of the efforts to make this condition recognizable and recognized, the organization has been working with experts and patients around the world towards a clinical case definition. Read the official report on that meeting here.
In the second seminar in the series, “Expanding our Understanding of the Post COVID-19 Condition: Towards a Clinical Case Definition,” there were several areas of particular interest to the ME/CFS community.
Dr. Janet V. Diaz (WHO) described the process for reaching the case definition. History of SARS-CoV-2 infection, Fatigue, cognitive dysfunction; shortening of breath, impact on everyday functioning and persistent symptoms that cannot be explained by alternative diagnosis currently make up the case definition. The overlap with case definitions of ME/CFS raises additional questions that would need to be resolved in the future. Potential confusion could be for instance when some people with Long-COVID are diagnosed as having ME/CFS with breathing issues that can be explained by a history of SARS-CoV-2 infection.
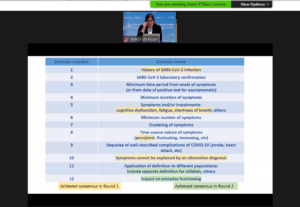
While there is a growing body of data describing the Post COVID-19 condition, with more than 2,000 scientific publications so far, a significant part of these studies looked at people who were hospitalized or had a severe course of the acute infection. Hannah Davis (Patient Led Research, the Long COVID Alliance) cautioned that the majority of people with Long-COVID were not hospitalized and didn’t experience respiratory symptoms. This perspective was shared by other researchers.
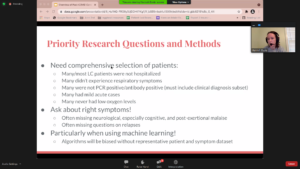
While the exact processes leading from the acute infection to the long-term symptoms are still not known, some important clues begin to emerge.
Dr. Akiko Iwasaki’s (Yale) research revealed that acute COVID-19, and possibly some viral remnants lead to the formation of a large number of antibodies that are directed at self targets. These autoreactive immune cells could explain many of the clinical symptoms of Long-COVID.
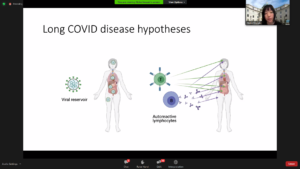
Ramsay Research Grant recipient Dr. Jarred Younger (U. of Alabama) drew on his prior research in ME/CFS and discussed the role that neuroinflammation, and specifically activation of microglia cells in the brain, play in Long COVID – and particularly the cognitive dysfunction and fatigue.
In the seminar, Oved alerted the audience to the recent publication by Solve M.E. Research Advisory Council member Dr. Anthony L. Komaroff and Dr. Ian Lipkin, making the case that insights from Myalgic Encephalomyelitis/Chronic Fatigue Syndrome may help unravel the pathogenesis of Post-Acute COVID-19 Syndrome.
We’ll keep you posted on future WHO meetings as they are announced.

