The Covering Life-saving Investigations Needed in Cancer and Other Life-threatening Conditions through Timely use of Resources for Easy and Affordable Treatment from Medicaid for Enrollees in Need Today Act (CLINICAL TREATMENT) Act, HR 913, introduced by Representatives Ben Ray Lujan (D-NM-03) and Gus Bilirakis (R-FL-12) guarantees coverage of the routine care costs of participation in an approved clinical trial for Medicaid enrollees with a life-threatening condition.
Medicare, private, and commercial payers already guarantee this coverage. Medicare has paid for these services since a 2000 National Coverage Decision. Private payers are required to provide coverage under the provisions of the Public Health Service Act section 2709 – enacted as part of the Affordable Care Act. Medicaid, which covers many of the nation’s most complex patients, should also guarantee this coverage.(1)
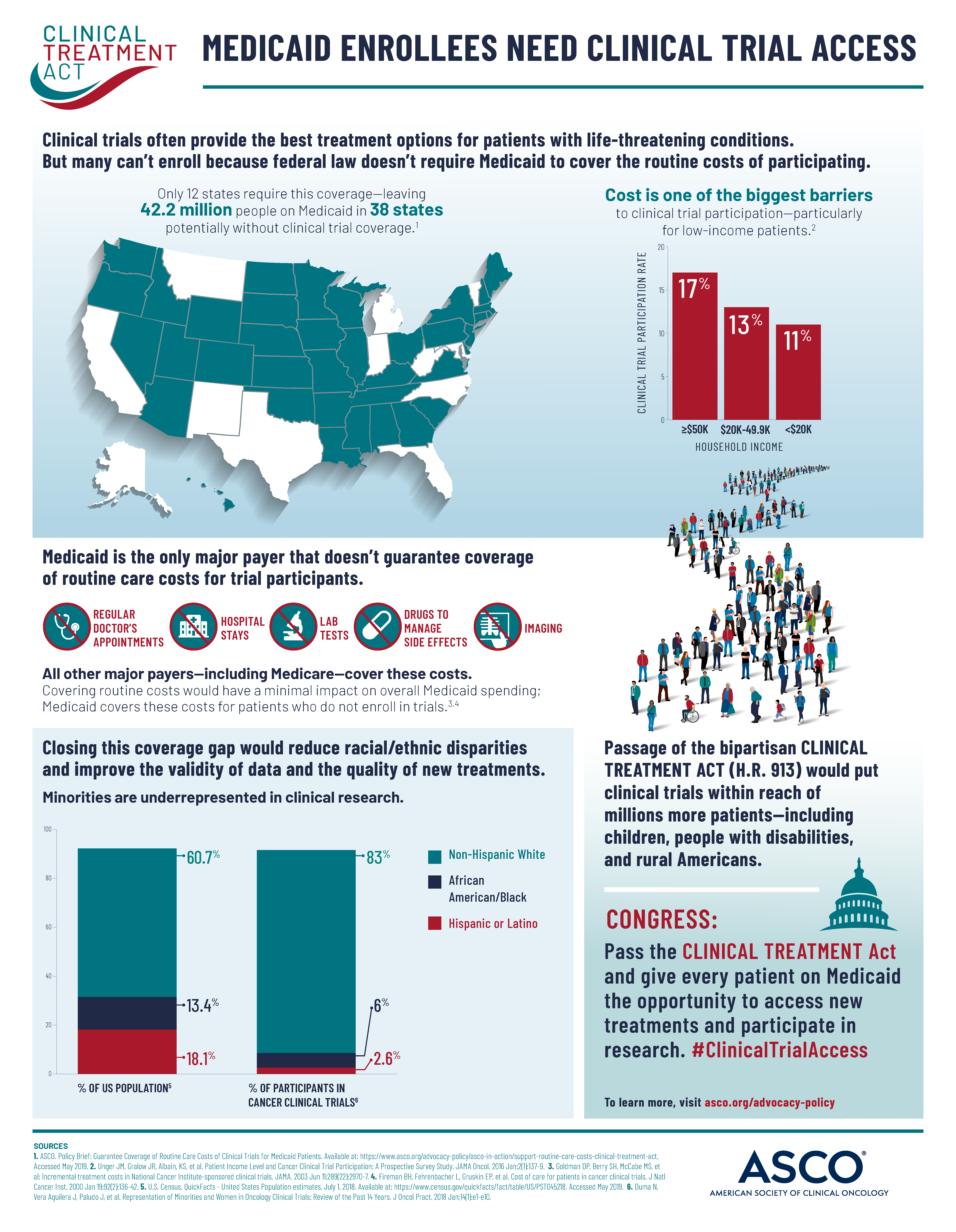
Medicaid insures nearly one-fifth of the U.S. population and is the last major payer that is not required by federal law to provide coverage of the routine costs of participation in a clinical trial. Removing the states that already guarantee this coverage, there are still approximately 42.2 million Medicaid enrollees without.
Clinical trial participation benefits cancer patients in ways that go beyond the value of the research data generated within the trial, and clinical trials often provide individuals with cancer with their best clinical option.
Improving representation improves the validity of clinical research data and quality of new treatments. Medicaid serves a large portion of under-represented minorities and ethnicities that are not well represented in clinical trial enrollment. Failure to address the coverage barrier that Medicaid patients face could further exacerbate existing disparities and prevents researchers from obtaining optimal results in clinical trials.
Providing coverage for the routine costs of clinical trials is affordable for states as several studies have demonstrated a minimal effect on overall care costs.(2) Because in most cases, this is coverage for care that patients would be receiving anyway. Routine care costs include the non-experimental costs of treating a patient who is participating in a clinical trial, such as physician visits and laboratory studies.
The cost of the investigational device or drug would still be covered by the trial sponsor.
1.These states are: Alaska, California, DC, Florida, Indiana, Maryland, Michigan, Montana, New Mexico, North Carolina, Texas, Vermont, and
West Virginia.
2. Impact of Clinical Trials on the Cost of Cancer Care. http://www.ncbi.nlm.nih.gov/pubmed/11329524
For a downloadable copy of HR 913, click here.
To read our letter of support for HR 913, click here.
For a downloadable copy of the infographic above, click here.